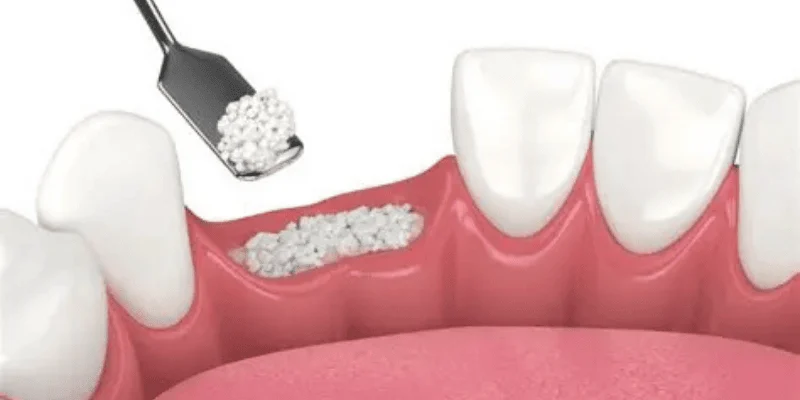
You want dental implants that feel stable and last for years, but bone loss can stand in the way. When a tooth goes missing, your jawbone can shrink, which makes implant placement harder. Bone grafting solves this problem by rebuilding the bone that implants need to stay secure.
Bone grafting for dental implants supports and restores lost jawbone, creating a strong base that allows the implant to bond and stay stable over time.
With enough healthy bone, implants can handle daily chewing and feel more like natural teeth. This step often makes the difference between an implant that lasts and one that fails.
You may be unsure about adding another procedure to your treatment plan. Learning how bone grafting works, when it helps, and what to expect can ease concerns and help you feel confident about your next steps.
Key Takeaways
- Bone grafting rebuilds the jawbone to ensure implants remain stable.
- Some implant cases need grafting due to bone loss.
- Grafting improves long-term implant strength and comfort.
Key Role of Bone Grafting in Dental Implant Success
Dental implants rely on a strong and stable jawbone to work as designed. Bone grafting rebuilds lost bone, improves healing, and helps your implant stay secure over time.
Why Bone Health Matters for Implants
Your jawbone holds the implant in place, much like soil holds a fence post. When you lose a tooth, the bone no longer gets regular pressure from chewing. This leads to jawbone loss through a process called bone resorption.
Bone grafting restores bone volume and strength before or during implant placement. It creates a firm base that can support dental implants under daily chewing forces. Without enough bone, the implant may shift or loosen.
Common causes of bone loss include:
- Missing teeth left untreated
- Gum disease
- Past dental infections or injuries
By rebuilding bone, grafting helps protect your bite, facial shape, and long-term oral health.
Importance of Osseointegration
Osseointegration is the process where the implant fuses with your natural bone. This bond allows the implant to act like a real tooth root.
Bone grafting supports osseointegration by encouraging bone regeneration around the implant. Healthy, dense bone grows into the implant surface and locks it in place. This step is critical for stability.
Bone grafts help by:
- Improving bone quality at the implant site
- Reducing movement during healing
- Supporting even pressure while chewing
Studies on the role of bone grafting in dental implant success show that strong bone greatly improves long-term implant results.
What Happens Without Enough Bone
Placing an implant without enough bone increases the risk of implant failure. The implant may not anchor well, which can lead to pain, infection, or loosening.
Without grafting, you may face:
- Delayed or failed healing
- Poor implant alignment
- Ongoing bone loss around the implant
In some cases, the implant cannot be placed at all. According to guidance on why bone grafting is needed for implants, grafting restores the bone needed for safe placement.
Bone grafting gives your implant the structure it needs to function and last.
Considering dental implants in New Market, VA? Schedule a consultation with Briggs Family Dental to learn how bone grafting can ensure stable, long-lasting implants.
When Bone Grafting Is Needed for Dental Implants
You may need bone grafting when your jawbone cannot hold an implant in a stable way. Bone loss after tooth removal, damage from gum disease or injury, and low bone strength can all affect implant success and timing.
Bone Loss Due to Tooth Extraction
After a tooth comes out, the bone under it starts to shrink. This process is called bone resorption, and it can begin within weeks. Without a tooth root to stimulate the area, your body absorbs unused bone.
If you wait too long to replace a missing tooth, jawbone loss can reduce height and width. That makes implant placement harder or unsafe. Many dentists suggest bone augmentation right after extraction to help prevent bone loss.
A bone graft placed at this stage can protect the socket and keep your options open.
Effects of Gum Disease and Trauma
Advanced gum disease can destroy bone around teeth. As infection spreads, it weakens support and leads to tooth loss. You may not feel pain at first, but damage can continue under the gums.
Injury to the face or jaw can also break or thin bone. Accidents, sports injuries, or past surgeries often cause uneven bone loss. In these cases, implants need extra support.
An oral surgeon or dentist may recommend grafting to rebuild damaged areas.
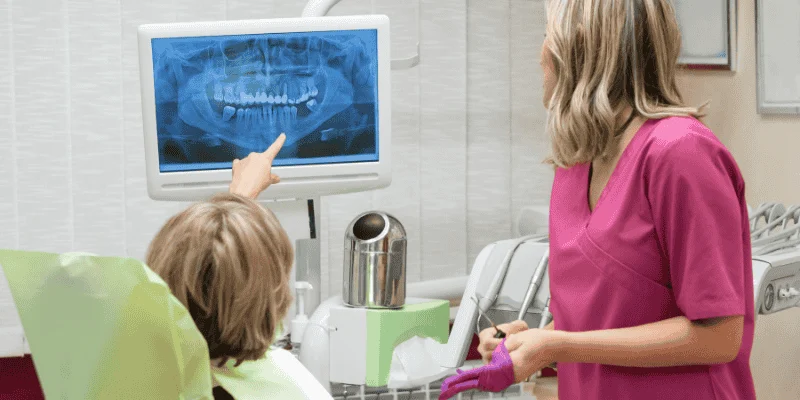
Assessing Bone Quality Before Implant Placement
Before placing dental implants, your dentist checks bone height, width, and density. X-rays or 3D scans show if your jaw can hold an implant without risk.
Common checks include:
| What Your Dentist Reviews | Why It Matters |
| Bone thickness | Prevents implant movement |
| Bone density | Supports long-term stability |
| Healing history | Affects success rates |
If scans show weak bone, grafting should be performed first. Nearly half of implant patients require this step, according to the findings. This planning step helps you avoid failure and delays later.
Types of Bone Grafts and Materials Used
Dental implants need strong bone to stay stable. Dentists choose graft materials based on where bone loss happened, how much bone you need, and how your body heals. Each option balances healing speed, availability, and comfort.
Autograft
An autograft, also called an autogenous bone graft, uses bone from your own body. Dentists often take it from your jaw, chin, or hip. This type brings living bone cells, which help new bone grow faster.
Your body accepts this graft well because it is your own tissue. That lowers the risk of rejection and supports solid bonding with the implant. Many dentists view it as the standard choice for larger defects.
The downside is the extra surgery. You may experience increased soreness and require more healing time. As a result, dentists typically reserve autografts for complex cases or significant bone loss.
Allograft and Xenograft
An allograft uses processed human bone from a donor. A xenograft uses animal bone, most often from cows or pigs. Both options avoid a second surgery site, which many patients prefer.
These graft materials act as a framework. Your natural bone grows into them over time. They work well for moderate bone loss and common implant cases.
Allografts and xenografts undergo rigorous cleaning protocols to reduce health risks. Some patients have ethical or personal concerns, which you should discuss with your dentist.
Research shows these materials integrate well when used correctly in dental care, as outlined in this overview of bone graft materials in dentistry.
Synthetic and Alloplast Options
Alloplast and synthetic bone graft materials come from lab-made sources like calcium phosphate or bioactive glass. These materials do not come from people or animals.
Dentists use them often for small defects or socket preservation. They provide a stable base that guides new bone growth. Your body slowly replaces the material with natural bone.
Synthetic options offer steady quality and wide availability. They do not carry disease risk, which reassures many patients. Some types may heal more slowly than natural bone. You can review common synthetic bone graft materials used in dentistry.
Quick comparison of common graft materials
| Graft type | Source | Key benefit |
| Autograft | Your own bone | Fast healing |
| Allograft | Human donor | No second surgery |
| Xenograft | Animal bone | Strong structure |
| Alloplast | Synthetic | No biological risk |
Have questions about bone grafting for dental implants or your treatment options? Contact our team today to get expert guidance and personalized recommendations for a secure, natural-looking smile.
Common Bone Grafting Procedures for Dental Implants
Different bone grafting procedures prepare your jaw to hold implants with strength and balance. Each method targets a specific type of bone loss and timing issue, so your dentist can match the procedure to your needs.
Socket Preservation
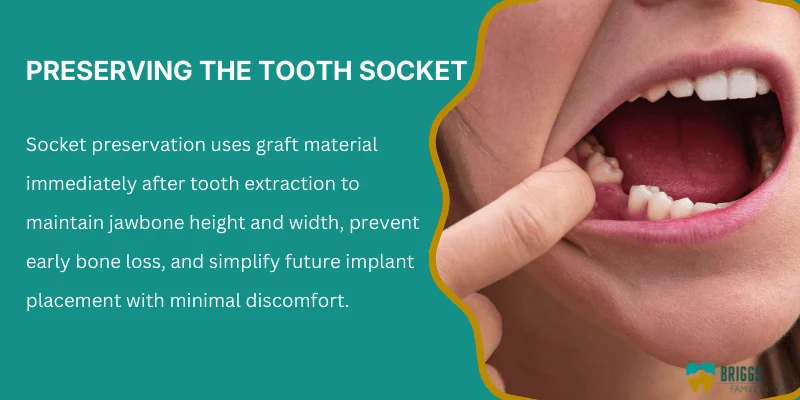
Socket preservation starts right after a tooth removal. Your dentist places graft material into the empty socket to keep the bone from shrinking. This step matters because bone loss can begin within weeks after extraction.
This dental bone graft procedure helps keep the jaw’s height and width stable. It often makes later implant placement simpler and more predictable. Many patients heal well with minimal discomfort.
Why socket preservation helps you:
- Keeps bone shape after extraction
- Reduces the need for later grafting
- Shortens the overall implant timeline
Ridge Augmentation
Ridge augmentation rebuilds areas where the jaw has already lost bone. Your dentist adds graft material to increase bone width, height, or both. This creates enough space to anchor an implant securely.
You may need this bone grafting procedure if tooth loss happened long ago or if gum disease caused bone damage. Healing can take several months, but it improves implant stability.
Ridge augmentation often addresses:
- Thin or uneven jawbone
- Collapsed ridges
- Poor implant positioning
This approach supports long-term success for bone grafts for dental implants.
Sinus Lift and Sinus Augmentation
A sinus lift, also called sinus augmentation, treats bone loss in the upper back jaw. Your dentist gently lifts the sinus membrane and places bone graft material underneath it. This creates space for implants near the molars.
You may need a sinus lift procedure if your sinuses sit too close to the jawbone. This often happens after years of missing upper teeth.
Key points about sinus augmentation:
- Common for upper jaw implants
- Requires careful planning
- Healing usually takes several months
This method plays a key role in sinus lift and sinus augmentation for implants.
Other Advanced Techniques
Some cases need advanced solutions when standard grafts are not enough. Techniques like guided bone regeneration use membranes to protect and shape new bone as it heals. Others rely on specialized graft materials chosen for your bone quality.
In rare cases, your dentist may discuss alternatives such as zygomatic implants, which anchor into cheekbone instead of jawbone. These options suit severe bone loss but require expert care.
Advanced options may include:
- Guided bone regeneration
- Block bone grafts
- Specialized implant designs
These methods appear in detailed guides on advanced bone grafting techniques for implant dentistry.
The Bone Grafting Process: What to Expect Before, During, and After
Bone grafting follows a clear path, from planning to healing. Each stage helps build stable bone so your dental implant can stay secure and support long-term oral health.
Consultation and Treatment Planning
Your dentist or oral surgeon starts with a full exam of your mouth and jaw. They review your health history and take X-rays or 3D scans to measure bone height and width. These images show where bone loss has occurred and how much grafting you need.
You also discuss the type of bone graft procedure that fits your case. Options may include donor bone or lab-made material, based on safety and healing goals. The provider explains timing, costs, and how grafting fits into your implant plan. This step sets clear expectations and lowers the risk of delays later.
Step-by-Step Procedure Overview
The bone graft procedure is performed during oral surgery, often in a single visit. The oral surgeon numbs the area, and some patients choose sedation for comfort.
The basic steps usually include:
- Cleaning and preparing the graft site
- Placing the bone graft material where the bone is thin
- Covering the graft with a membrane to protect the healing
- Closing the area with small stitches
Most procedures take under 90 minutes. You go home the same day with care instructions. The goal is to create a firm base that can hold an implant without shifting.
Planning a visit to our New Market, VA, clinic? Complete the new patient forms online to streamline your consultation and discuss implant planning in a stress-free environment.
Bone Graft Recovery and Healing Timeline
Dental bone graft recovery happens in stages. In the first few days, swelling and soreness are common. You control this with cold packs and prescribed medication.
Soft tissue often heals within one to two weeks. During this time, you may eat soft foods and limit activity. Bone graft recovery takes longer than it feels. The graft slowly joins your natural bone over several months.
Many people wait 3 to 9 months before implant placement. Your oral surgeon checks healing progress with follow-up visits before moving forward.
Tips for Successful Healing
You play a big role in how well the graft heals. Follow instructions closely and protect the surgical area.
Key healing tips include:
- Avoid smoking, which slows bone growth
- Keep the area clean without brushing directly on stitches
- Eat soft, nutrient-rich foods
- Take all medications as prescribed
Call your dentist if you notice unusual pain or swelling. Careful healing supports a strong implant and protects your long-term oral health.
Long-Term Benefits and Outcomes of Bone Grafting for Dental Implants
Bone grafting builds the bone you need to support dental implants, protect your jaw, and keep your smile stable. It also plays a clear role in comfort, function, and long-term oral health.

Supporting Stable Implants
Bone grafting gives your implant a solid base so it can bond with your jaw. This bond helps the implant stay firm when you chew and speak. Without enough bone, implants can loosen over time.
Studies show that bone regeneration improves implant stability and lowers the risk of failure. A review of implant outcomes found strong survival rates when guided bone regeneration supported placement, as described in this research on bone graft success and implant survival.
Key ways bone grafting helps stability include:
- Better load support during chewing
- Reduced movement around the implant
- Improved bone-to-implant contact
These factors work together to support dental implants for daily use over many years.
Preserving Jawbone and Facial Structure
After tooth loss, your jawbone can shrink. Bone grafting helps prevent bone loss by filling gaps and encouraging new bone growth. This process protects the natural shape of your jaw.
When bone volume stays stable, your facial features look more balanced. Sunken areas around the mouth become less likely. Many dental specialists stress this benefit when explaining the importance of bone grafting for dental implants.
Bone grafting helps by:
- Slowing jawbone shrinkage
- Supporting nearby teeth
- Keeping your bite aligned
These changes support both appearance and function without adding complex care needs.
Enhancing Oral Health and Quality of Life
Bone grafting supports long-term oral health by creating a cleaner, more stable oral environment. Stable implants are easier to care for than loose teeth or removable options.
A strong jawbone lowers the risk of gum problems and uneven pressure on nearby teeth. This guidance appears often in patient-focused explanations of bone grafting for dental implants.
You may notice practical benefits like:
- Easier chewing of firm foods
- Clearer speech
- More confidence when smiling
These outcomes help you maintain daily comfort while protecting your oral health over time.
Visit Briggs Family Dental in New Market to explore how bone grafting can strengthen your jaw and support long-lasting, natural-feeling dental implants.
Frequently Asked Questions
These answers address costs, recovery time, warning signs, and planning steps to consider before moving forward with bone grafting and dental implants.
What are the typical costs associated with dental bone graft procedures?
Dental bone graft costs often range from $800 to $2,500 per graft, based on the graft type and treatment area. Location and the surgeon’s experience can also change the price.
This general range aligns with common estimates explained in this guide on dental bone graft cost and success rates.
What can I expect during the bone graft healing process?
You can expect swelling, mild pain, and tenderness for several days after surgery. Most people manage discomfort with basic pain medicine and rest.
Full healing usually takes three to six months, depending on graft size and material. This timeline matches what many patients experience during dental bone graft recovery.
Are there any tips to help accelerate the healing after a bone graft for an implant?
You can support healing by eating soft foods and avoiding chewing near the graft site. You should also avoid smoking, as it slows bone growth.
Follow your dentist’s cleaning and medication instructions closely. Consistent care improves outcomes, as outlined in this overview of bone graft healing and implant preparation.
How much financial investment is needed for two dental implants with bone grafting?
Two dental implants with bone grafting typically cost several thousand dollars per tooth, depending on the grafting required and theimplant type. The total may increase if sinus lifts or advanced grafts are required.
This combined treatment is commonly discussed in guides on dental implant bone graft procedures and pricing.
What is the recommended time frame between a bone graft and placing a dental implant?
Most dentists recommend waiting three to six months before placing an implant. This allows the grafted bone to fully bond with your jaw.
Your dentist confirms readiness using X-rays and exams, as explained in this bone grafting timeline for dental implants.
What indicators should I watch for to identify a failed bone graft?
Signs may include ongoing pain, worsening swelling, pus, or a loose graft site. Fever or a persistent bad taste can also signal trouble.
If you notice these issues, contact your dentist right away. Early treatment improves outcomes, according to this overview of bone graft risks and warning signs.