Losing a tooth can affect how you eat, speak, and feel about your smile. Many people wonder if dental implants are a good option to replace missing teeth. Dental implants are considered safe for most people and have been used successfully for decades to restore both function and appearance.
The safety of dental implants depends on several factors, including your overall health, the skill of your dental provider, and how well you care for them afterward. Like any surgical procedure, implants come with some risks, but serious complications are rare when the procedure is done correctly.
Understanding what makes you a good candidate, what to expect during the procedure, and how to care for your implants can help you make an informed decision. This guide will walk you through everything you need to know about dental implant safety so you can move forward with confidence.
Key Takeaways
- Dental implants are safe medical devices for most people when placed by a qualified dental provider
- Good candidates have healthy gums, adequate jawbone, and commit to proper oral hygiene after the procedure
- Following your dentist’s aftercare instructions and maintaining regular dental visits helps ensure long-term implant success
How Safe Are Dental Implants?
Modern dental implants have proven to be one of the safest and most reliable options for tooth replacement, with success rates consistently above 90% and millions of procedures completed successfully each year.
Long-Term Success Rates and Safety Statistics
When you’re considering dental implants as a safe option, the numbers tell a reassuring story. Long‑term studies show dental implant survival rates around 90–95% over a 10‑year period, meaning most implants remain stable and functional for many years after placement.
These statistics mean that most people who get dental implants will still have them functioning well a decade later. Your individual results depend on several factors, including your overall health, bone quality, and the experience of your dental team.
The safety of dental implants has improved significantly with advances in technology and surgical techniques. Complications do occur, but they remain relatively uncommon when proper protocols are followed.
Factors That Affect Implant Safety
Your personal health plays a major role in implant safety. Smoking significantly increases your risk of implant failure and infection. If you have uncontrolled diabetes, certain immune conditions, or osteoporosis, your risk may be higher.
The quality and amount of your jawbone matters too. If you’ve been missing teeth for a long time, your bone may have shrunk, making the procedure more complex.
Your oral hygiene habits directly impact implant safety. Poor dental care after surgery raises your infection risk. The complexity of your case also matters. A single tooth implant typically carries lower risk than multiple implants or full-arch reconstructions.
Your dentist’s experience and training affect outcomes significantly. Providers who use 3D imaging and computer-guided placement generally report better results and fewer complications.
Comparing Dental Implants to Other Tooth Replacement Options

Dental implants offer distinct safety advantages over bridges and dentures. Unlike bridges, implants don’t require grinding down healthy adjacent teeth, which preserves your natural tooth structure.
Compared to bridges:
- Implants don’t stress neighboring teeth
- They last longer (often 20+ years vs. 10-15 years for bridges)
- They preserve jawbone instead of allowing bone loss
Compared to dentures:
- Implants stay firmly in place without slipping
- They prevent the bone loss that occurs with dentures
- No adhesives or removal needed for cleaning
Implants feel and function more like your natural teeth. They let you eat, speak, and smile with confidence. While the initial surgical procedure carries more risk than getting a bridge or denture fitted, the long-term benefits and durability often make implants the safest choice for your overall oral health.
Considering dental implants? Visit Briggs Family Dental in New Market, VA, to explore your options and get personalized care tailored to your needs.
Who Is a Good Candidate for Dental Implants?
Most people with missing teeth can get dental implants, but your success depends on meeting certain health requirements. Your jawbone needs to be strong enough to support the implant, and your gums should be healthy and free from disease.
Health and Oral Requirements
Your overall health plays a big role in whether dental implants are right for you. You need to be healthy enough to undergo oral surgery and heal properly afterward.
Key health factors include:
- Being free from uncontrolled diabetes or autoimmune diseases
- Not taking medications that slow bone healing
- Having a strong immune system
- Being old enough that your jaw has stopped growing (usually age 18 or older)
Your oral health matters just as much. You should have healthy gums with no active infections or untreated cavities. Good candidates maintain excellent oral hygiene through regular brushing and flossing.
Smoking can reduce your chances of implant success because it slows healing and affects blood flow to your gums. Your dentist will likely recommend quitting before the procedure.
Jawbone and Bone Grafting Considerations
Your jawbone needs enough density and volume to hold the implant securely. The titanium post that acts as your tooth root must fuse with strong, healthy bone.
If you’ve been missing teeth for a while, your jawbone may have gotten thinner over time. This doesn’t automatically disqualify you. Modern bone grafting procedures can rebuild your jawbone to the right thickness.
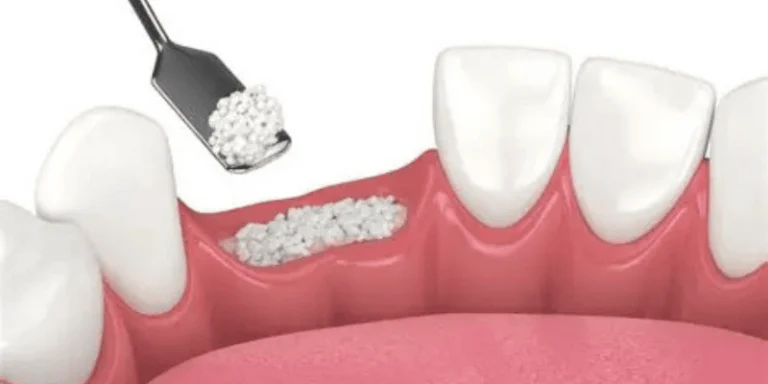
Bone graft options include using bone from another part of your body, donor bone, or synthetic materials. The bone grafting process adds several months to your treatment timeline because the new bone needs time to heal and strengthen before receiving an implant.
Your dentist will use X-rays or CT scans to measure your bone density and create a personalized treatment plan based on your specific needs.
Impact of Gum Disease and Oral Health
Gum disease is one of the biggest obstacles to getting dental implants. Active gum infections can cause implants to fail because bacteria prevent proper healing and bone integration.
You must treat any existing gum disease before implant surgery. This might include deep cleaning procedures, antibiotics, or other treatments to eliminate infection. Healthy gums provide the foundation that supports your implant long-term.
Your oral health routine after getting implants is just as important as before. You’ll need to commit to brushing twice daily, flossing around your implants, and visiting your dentist regularly. Poor oral hygiene after surgery can lead to peri-implantitis, an infection similar to gum disease that can cause your implant to fail.
Regular dental checkups help catch any problems early and keep your implants functioning properly for decades.
Understanding the Dental Implant Procedure
The dental implant procedure involves multiple stages over several months, with careful planning and advanced technology ensuring safe and successful results. Each step requires specific materials and techniques to help your new tooth function like a natural one.
Pre-Surgical Assessment and Planning
Your dentist will start with a thorough examination of your mouth and jawbone before any surgery begins. This assessment includes digital imaging like X-rays or CT scans to see the exact condition of your bone structure. These images help your dental team plan where to place the titanium post for the best results.
Your dentist will also review your medical history during this phase. They need to know about any medications you take or health conditions you have. This information helps them decide if you need any special preparations before surgery.
Some patients need additional procedures first. You might need a bone graft if your jawbone isn’t thick enough to support the implant. Others may need teeth removed before the implant placement can begin.
Overview of Implant Placement and Surgery
The implant surgery involves general or local anesthesia to keep you comfortable during the procedure. Your oral surgeon will make a small cut in your gum to access the jawbone underneath. They then drill a hole and place the titanium post into your jawbone.
This post acts as the root of your new tooth. Your gums will be stitched closed over the post, and then you wait several months for healing. During this time, your bone grows around the post to hold it firmly in place.
After healing, you return for the next step. Your surgeon attaches a connector piece called an abutment to the post. The crown (your artificial tooth) then attaches to this abutment. The entire dental implant procedure takes several months from start to finish.
Role of Materials and Technology
Dental implant systems must be approved by the FDA, which follows international standards for safety. The materials used in your implants go through careful testing before approval. Most dental implants use biocompatible materials that work well with your body.
Titanium implants are the most common choice because this metal bonds naturally with bone. The titanium post becomes a stable foundation for your new tooth over time. Some implants use ceramic materials, but titanium remains the standard option.
Modern technology has made implant surgery more precise and safer. Digital imaging lets dentists see exactly where to place implants before surgery starts. Sterile surgical protocols protect you from infection during the procedure. These advances help ensure your implants last for many years.
Ready for a consultation? At Briggs Family Dental in New Market, VA, we use the latest technology and high-quality materials to provide you with safe, long-lasting implants. Contact us today to get started!
Potential Risks and How They Are Managed
Dental implant procedures carry some risks, but most complications can be prevented or treated effectively with proper planning and care. Understanding infection prevention, implant failure causes, and potential nerve or sinus issues helps you prepare for a successful outcome.
Preventing Infection and Promoting Healing
Infection around your implant can lead to peri-implantitis, which causes inflammation and bone loss. You’ll notice early warning signs like swelling, bleeding when you brush, or a bad taste in your mouth.
Your dentist will give you specific cleaning instructions to follow after surgery. Good oral hygiene is your best defense against infection.
Steps to prevent infection:
- Brush gently around the implant site
- Use prescribed antibacterial mouthwash
- Avoid smoking during healing
- Take antibiotics only if prescribed
- Attend all follow-up appointments
If infection does develop, your dentist can treat it with professional cleaning, antibiotics, or laser therapy. Catching problems early makes treatment much easier and protects your implant from failing due to untreated peri-implantitis.
Implant Failure: Causes and Solutions
Implant failure happens when your jawbone doesn’t bond properly with the titanium post. This process is called osseointegration, and it’s essential for your implant to work long-term.
Early failure occurs within the first few months. Late failure can happen years later. Smoking, uncontrolled diabetes, and poor bone quality increase your risk significantly.
Common causes of implant failure:
- Insufficient bone density or volume
- Smoking or tobacco use
- Infection or inflammation
- Too much movement during healing
- Medical conditions affecting bone health
Your dentist uses X-rays and clinical exams to catch problems early. If your implant fails, you may need bone grafting before trying again. Some patients require a different implant type or staged treatment to improve outcomes when risk is higher.
Nerve, Tissue, and Sinus-Related Complications
Nerve damage can cause numbness or tingling in your lip, chin, or tongue. This happens when implants are placed too close to nerves in your jaw. Most minor nerve issues resolve within a few weeks.
Sinus issues occur when upper jaw implants penetrate the sinus cavity. Your dentist may recommend sinus lift procedures to create enough bone height before placing your implant.
Warning signs that need attention:
- Persistent numbness lasting more than two weeks
- Pain when chewing or biting
- Fluid leaking from your nose
- Pressure or congestion in your sinuses
Modern 3D imaging helps your dentist map nerve locations and plan sinus lift procedures safely. Guided surgery and computer navigation reduce the risk of nerve injury during placement. If you experience lasting numbness or sinus problems, contact your dentist right away for evaluation.
Aftercare and Improving Implant Safety
Taking care of your dental implants after surgery directly affects how well they heal and how long they last. Good daily cleaning habits and regular dental visits help prevent problems and keep your implants working properly for years.
Maintaining Good Oral Hygiene
Your oral hygiene routine becomes even more important once you have dental implants. You need to brush at least twice daily using a soft-bristled toothbrush to clean around the implant without causing damage.
Flossing daily removes food particles and plaque from areas your toothbrush can’t reach. Use unwaxed tape or implant-specific floss to clean gently between your implants and natural teeth.
Proper aftercare plays a huge role in how well your implants heal after surgery. During the first few weeks, you should avoid hard or sticky foods that could disturb the healing process.
Rinsing with an antimicrobial mouthwash helps reduce bacteria around your implant sites. Your dentist may recommend specific products that work best with your personalized treatment plan.
Long-Term Monitoring and Checkups

Regular dental checkups let your dentist spot potential issues before they become serious problems. You should visit your dentist every six months for professional cleanings and examinations.
Routine exams and cleanings are crucial for maintaining the strength and stability of your implants. Your dentist will check for signs of infection, bone loss, or loosening during these visits.
X-rays taken during checkups show how well the implant has fused with your jawbone. These images help your dentist monitor your oral health and catch any changes early.
Professional cleanings remove hardened plaque that regular brushing can’t eliminate. Your dental team uses special tools designed to clean implants without scratching or damaging them.
Ensure the long-term success of your dental implants. Schedule your next checkup with Briggs Family Dental in New Market, VA, and keep your smile healthy for years to come!
Frequently Asked Questions
People considering dental implants often have similar concerns about candidacy, costs, procedures, and potential complications. Understanding the materials used and what to expect can help you make an informed choice about tooth replacement.
What should I consider before deciding to get dental implants?
Your overall health plays a major role in whether you’re a good candidate for dental implants. Certain conditions like uncontrolled diabetes can affect healing and increase infection risk.
Smoking is another important factor to consider. It can slow down the healing process and reduce the long-term success of your implant.
You should ask your dental provider what brand and model of implant system they plan to use. Keep this information in your records for future reference.
The healing process can take several months or longer. During this time, you’ll typically have a temporary abutment in place of the tooth while the implant body fuses with your jawbone.
Can dental implants have adverse effects, and what might they be?
Dental implants can cause damage to surrounding natural teeth during placement. Injuries to nearby tissues like sinus perforation can also occur during surgery.
You might experience inadequate function where your teeth don’t feel like they bite together normally. Sometimes the abutment screw can loosen, making the tooth feel loose or like it’s twisting.
Implant body failure can happen due to systemic infection, which is more common in patients with uncontrolled diabetes. Local infection in the bone and gums supporting the implant can also cause failure.
Post-surgical numbness may occur if nerves are damaged during the procedure. Some patients find it difficult to clean around the implant, which can lead to poor oral hygiene and complications.
What are the typical costs involved in getting a dental implant?
The cost of dental implants varies widely depending on several factors. Single tooth implants typically range from $1,500 to $6,000 per tooth.
The price depends on the complexity of your case and where you live. Additional procedures like bone grafting or sinus lifts will increase the total cost.
Your dental provider’s experience level can also affect pricing. While implants may seem expensive upfront, they often provide better long-term value compared to other tooth replacement options.
Most dental insurance plans don’t cover the full cost of implants. You may need to explore financing options or payment plans with your dental office.
How does the dental implant procedure work step by step?
The first step involves a consultation where your dentist evaluates your oral health and jawbone density. X-rays or CT scans help determine if you have enough bone to support an implant.
Your dentist surgically places the implant body into your jawbone where the tooth root used to be. This metal post acts as an artificial tooth root and needs time to fuse with the bone.
The healing period typically lasts several months. During this time, a process called osseointegration occurs where the bone grows around the implant.
Once healing is complete, your dentist attaches an abutment to the implant body. This piece connects the implant to the artificial tooth or crown that will be visible in your mouth.
The final step involves placing the custom-made crown onto the abutment. Your dentist makes sure it matches your natural teeth in color and shape.
What are the most common complications with dental implants?
Infection at the implant site is one of the most frequent complications. This can happen during or after surgery if bacteria enter the area around the implant.
Nerve damage can occur if the implant is placed too close to a nerve. This may cause pain, numbness, or tingling in your teeth, gums, lips, or chin.
Implant failure happens when the implant doesn’t properly fuse with the jawbone. Smoking and certain health conditions increase this risk significantly.
Bone loss around the implant can develop over time. This often results from poor oral hygiene or untreated gum disease.
The abutment screw can sometimes loosen, causing the crown to feel unstable. This usually requires a simple fix by your dentist.
What are the different types of dental implants available?
Endosteal implants are the most common type and are placed directly into the jawbone. These titanium screws look like small posts and work well for most patients who have adequate bone height.
Subperiosteal implants sit on top of the jawbone but under the gum tissue. These are used when you don’t have enough healthy jawbone and don’t want to undergo a bone augmentation procedure.
Most dental implant systems use titanium or zirconium oxide materials. These materials follow international safety standards and have well-known safety profiles.
Some implants use other materials like gold alloys, cobalt-based alloys, or ceramic materials. Your dentist will recommend the best type based on your specific needs and bone structure.
Mini dental implants are smaller in diameter than traditional implants. They’re often used to stabilize dentures or in areas where there’s limited space.