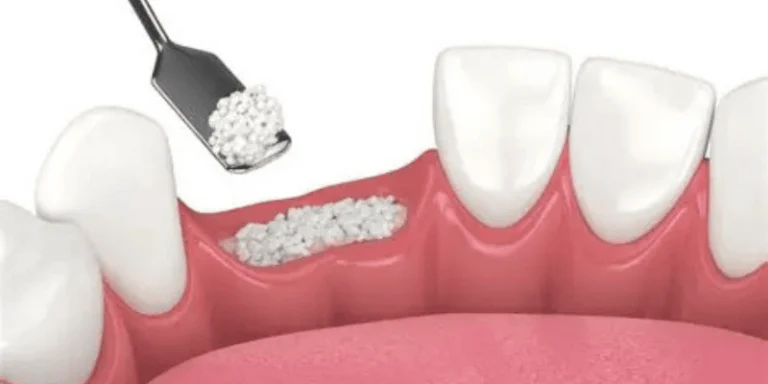
Dental implants are a popular way to replace missing teeth and restore your smile. While they usually work well, it’s important to know that there are some risks involved.
Common problems include infections, nerve damage, and issues with how the implant bonds to your bone. Sometimes, habits like teeth grinding or poor oral hygiene can cause complications.
By taking care of your implants and following your dentist’s advice, you can lower the chances of problems. Knowing what to expect and how to protect your dental implants makes a big difference in their success.
This post will guide you through the main risks and show you simple ways to keep your implants healthy and strong.
Key Takeaways
- Dental implants have risks but can be successful with proper care.
- Infection and bone problems are common causes of implant issues.
- Good habits and regular checkups help prevent complications.
Understanding Dental Implants and Their Benefits
Dental implants offer a strong, long-lasting way to replace missing teeth. They are designed to work closely with your jawbone to support natural-looking teeth.
You can expect a solution that not only restores your smile but also helps maintain your oral health.
How Dental Implants Work
Dental implants are small titanium posts surgically placed into your jawbone by an implantologist. This surgery creates a stable base that acts like a natural tooth root.
Over time, your bone grows around the implant in a process called osseointegration, locking it firmly in place. After healing, the implant supports a crown, bridge, or denture that looks and functions like your natural teeth.
This setup helps restore chewing ability and prevents jawbone loss, which often happens after missing teeth. The implant fuses directly with your bone, making it a sturdy and reliable replacement.
Why Success Rates Are High
The success of dental implants is linked to careful planning and precise placement. Your implantologist will assess your jawbone health, sometimes using 3D scans, to ensure the implant will fit well and avoid nearby nerves or sinuses.
Proper technique reduces healing problems and implant failure. Materials also play a role.
Titanium is biocompatible, causing minimal reaction from your body. With good oral hygiene and regular dental visits, implants can last many years.
Clinical evidence supports these outcomes. A large data analysis found dental implants have an overall survival rate of approximately 97.79%, with a failure rate of only about 2.21%, when proper planning, placement, and long-term care are followed.
Benefits Over Other Tooth Replacement Options
Compared to dentures or bridges, dental implants provide several clear advantages. They don’t require altering your nearby healthy teeth, preserving your natural smile.
Since implants fuse directly with your bone, they feel more natural and secure. Implants also help keep your jawbone healthy by preventing bone loss.
Dentures, on the other hand, can speed bone shrinking because they only sit on the gums. With implants, you avoid slipping or discomfort that often comes with removable dentures.
Finally, dental implants usually last much longer and improve your ability to speak and eat comfortably.
Common Risks and Complications of Dental Implants
When you get dental implants, there are a few risks you should watch out for. Some problems happen soon after surgery, while others might develop over time.
Knowing about these issues can help you spot signs early and take action to keep your implant healthy.
Peri-Implantitis and Infection
Peri-implantitis is a common and serious problem. It’s an infection that causes inflammation and bone loss around your implant.
If left untreated, it can make your implant loose and even lead to failure. You might notice swelling, redness, pain, or pus near the implant site.
Infections can also happen right after surgery. Preventive antibiotics and good oral hygiene can reduce this risk.
Using a medicated mouthwash and keeping your mouth clean are very important if you want to avoid infections. Smoking raises the chance of peri-implantitis, so quitting before and after surgery helps protect your implant.
Implant Failure and Rejection
Implant failure means your implant doesn’t properly fuse with your jawbone. This can happen early, usually within six months, or later on.
Failed osseointegration is often the main cause. You might feel your implant is loose or painful.
Certain health issues, like uncontrolled diabetes or smoking, increase failure risks. Early failure usually requires removal of the implant, followed by healing before a replacement can be placed.
Your dentist may need to do a bone graft. Keeping chronic conditions under control and following care instructions lowers your chances of this happening.
Nerve Injury and Altered Sensation
Nerve injury happens when nerves near your implant get damaged during surgery. This can cause numbness, tingling, or a burning feeling in your lip, chin, or tongue.
Sometimes the feeling comes back on its own, but other times it needs treatment. Your dentist uses scans to avoid nerves during placement, but injury can still happen.
If you notice unusual numbness lasting longer than eight hours or if it gets worse, contact your dentist quickly. Early treatment can often reduce permanent damage and improve healing.
Ongoing numbness or tingling should be evaluated promptly. Schedule a visit with Briggs Family Dental in New Market, VA, to assess nerve health and prevent long-term complications.
Bone-Related Issues and Sinus Complications
When getting dental implants, your jawbone’s health plays a big role. If your bone is weak or missing, it can cause problems.
Also, if implants are placed near the sinuses in your upper jaw, special care is needed to avoid sinus troubles.
Bone Loss and Bone Density Concerns
Bone loss means your jawbone shrinks or becomes less dense over time. This often happens after tooth loss because the bone no longer gets used.
Clinical research shows that within the first 6 months after a tooth is removed, jawbone resorption can be significant, with horizontal bone loss ranging from 29–63% and vertical bone loss from 11–22%.
Signs you might notice include changes in your bite, difficulty chewing, or changes in facial shape. Low bone density can make it hard for implants to stay stable.
Your implant needs a strong jawbone for support. If your bone is too thin or soft, the implant might fail or loosen.
Your dentist will check bone density before the procedure. In some cases, they may recommend ways to strengthen your bone or delay implants until your bone improves.
Sinus Issues with Upper Jaw Implants
When placing implants in the upper back jaw, the maxillary sinuses are close by. Sometimes, implants can accidentally poke into the sinus cavity.
This can cause sinusitis (sinus infection) or irritation. You might experience symptoms like nasal congestion, pain around your nose or forehead, or a stuffy feeling after implant surgery.
These need attention to prevent lasting problems. Studies show implant survival isn’t dramatically lowered if an implant enters the sinus slightly, but there is a higher chance of minor issues like sinus membrane thickening.
Your dentist will plan carefully to avoid these problems.
Bone Grafting and Sinus Lift Procedures
If your jawbone lacks enough height for an implant near the sinus, bone grafting or a sinus lift may be needed. Bone grafting adds new bone material to strengthen and build up weak areas.
A sinus lift raises the sinus floor to create room for bone and the implant. There are two main types: lateral window and transalveolar (crestal) approaches.
Both procedures improve implant stability and reduce the risk of sinus complications. Healing time is longer, but success rates are high.
Your dentist will explain which option best fits your bone condition and implant plans.
Schedule a consultation with Briggs Family Dental in New Market, VA, to see whether bone grafting or a sinus lift is needed before implant placement.
Mechanical and Prosthetic Failures
There are clear risks that can cause your dental implant to fail, especially related to its parts and how they hold together. These problems may affect your implant’s stability and how well your crowns, bridges, or fixtures work over time.
Mechanical Failure of Implants
Mechanical failure happens when parts of your implant break, loosen, or stop working properly. The most common issue is abutment screw loosening, which can happen in about 16% of cases.
This looseness can make your implant unstable and uncomfortable. In some cases, screws or implants themselves might fracture, though this is less common.
You might notice your implant feels loose or moves when it shouldn’t. Early detection is key because a loose implant can often be saved if treated quickly.
Mechanical failures happen more often in the first nine years after placement but tend to decrease later. Certain factors raise the chance of mechanical failure, like implant placement in the upper jaw (maxilla), where failures are about 4.6 times more likely than in the lower jaw (mandible).
Taking care of your implant and visiting your dentist regularly helps you catch these problems early and avoid bigger repairs.
Problems with Crowns, Bridges, and Fixtures
Your implant’s prosthetic parts, such as crowns, bridges, and fixtures, can also run into problems. Common issues include wear, breakage, and de-cementation of crowns or frameworks.
These failures can cause discomfort and affect your ability to chew properly. Poor maintenance and not following care instructions can increase the risk of these problems.
For example, if your implant-supported denture clips or attachments wear out, they might lose retention, making your prosthesis loose or unstable. This happens in up to 30% of cases with overdentures.
Choosing the right materials and having a proper prosthetic plan can reduce these risks. Regular dental checkups allow your dentist to spot any signs of damage early and fix or replace parts before they fail completely.
Managing your oral hygiene well also helps protect your prosthetic components from damage.
Key Factors That Increase Dental Implant Risks
Certain personal and medical factors can raise the chances of problems with dental implants. Knowing these can help you work with your dentist to reduce risks and improve your chances of a smooth recovery.
Patient-Related Risk Factors
Your daily habits and oral health play a big role in how successful your implant will be. Poor oral hygiene can cause infections around the implant site, which may lead to implant failure.
Smoking is another major risk. It reduces blood flow to your gums, slowing healing and increasing the chance of complications.
If you smoke, quitting before your implant can improve outcomes. Bone health is critical.
If you have low bone density or bone loss in your jaw, the implant may not anchor well. Your dentist or a specialist like a periodontist may suggest bone grafting to improve stability.
Maintaining regular check-ups and cleanings after surgery keeps your mouth healthy and lowers risks over time.
Medications and Medical History
Certain medications and health conditions affect how well your body handles implants. Bisphosphonates, used for bone diseases, can increase the risk of jaw bone problems after surgery.
Conditions like diabetes need to be well controlled. High blood sugar levels can slow healing and raise infection risk.
If you have a history of radiation therapy to your head or neck, it can impact bone healing and raise implant failure chances. Be sure to share your full medical history with your oral surgeon or oral and maxillofacial surgeon during your consultation.
This helps them design a safer treatment plan for you.
Importance of Pre-Op Evaluation
A thorough pre-op evaluation is key to minimizing risks. Your surgeon will review your medical history and perform tests to check bone quality and quantity.
CBCT scans (3D imaging) give a clear view of your jawbone structure, nerves, and sinuses. This detailed picture helps the surgeon place implants precisely while avoiding complications.
Guided surgery, which uses this imaging to plan and guide implant placement, increases accuracy. It lowers the chance of nerve injury or improper placement.
By investing time in this evaluation, you can avoid many common problems and improve your overall implant success.
How to Prevent Dental Implant Complications and Ensure Longevity
Keeping your dental implants healthy takes good choices and care before, during, and after the procedure. You need to pick the right expert, prepare well for surgery, and stick to a strong daily routine to protect your new teeth.
Choosing the Right Dental Professional

Your implant’s success depends a lot on who you choose for the job. Look for a dental professional called an implantologist.
They have special training in placing implants and understand your unique needs. Don’t be afraid to ask about their experience, how many implants they’ve placed, and if they use modern tools like guided surgery.
This technology helps plan the implant’s exact spot, reducing the risk of mistakes. A skilled implantologist will also check your oral health and bone strength before starting.
If needed, they might recommend treatments like bone grafts or gum care to build a strong foundation. Picking a pro who listens and answers your questions makes it easier to trust the process and follow care instructions.
Preparation and Surgical Techniques
Before surgery, you may need X-rays or 3D scans to map out your jawbone and nerves. This helps avoid damage during implant placement.
The dentist should explain the entire procedure, including any risks and how they plan to prevent them. During the surgery, the right techniques matter.
The dentist must keep the area clean and avoid placing the implant too close to nerves or sinuses. Using guided surgery tools can improve precision.
After the implant is in place, waiting for the bone to fuse naturally is key. Avoid putting pressure on the implant while healing, which could cause failure.
Post-Operative Care and Maintenance
After surgery, your job is to keep the implant site clean to prevent infections. Follow all post-op care rules, like eating soft foods and avoiding smoking.
Brush gently around the implant and floss daily with special tools like interdental brushes to reach tight spots. Using an antimicrobial mouthwash can reduce bacteria and lower your risk of gum disease around the implant.
Regular dental check-ups are vital to spot early problems like inflammation or bone loss. Your dentist can also professionally clean the area to keep everything healthy.
If you notice pain, numbness, or unusual swelling, report it right away.
Stay on track with healing and long-term implant health. Schedule a follow-up visit with Briggs Family Dental in New Market, VA for ongoing care and professional monitoring.
Frequently Asked Questions
Dental implants can last a long time, but it’s important to know about side effects and complications. You should also think about the costs, types, and what the process looks like before you decide.
What are the possible long-term side effects of dental implants?
Some long-term side effects include inflammation around the implant, called peri-implantitis. This can cause bone loss and implant failure if untreated.
Rarely, you might experience nerve damage that causes numbness or tingling. Good dental care and follow-ups reduce these risks.
Can dental implants negatively affect my life, and how can I prevent that?
Most people live without problems, but infections or implant failure can happen. These might cause pain, swelling, or difficulty chewing.
Avoid smoking and follow your dentist’s advice to keep your implants healthy. Good oral hygiene is key to prevention.
What should I consider before deciding to get dental implants?
Consider your overall health, bone density, and any medical conditions. Some medicines and smoking can impact healing.
Ask about the experience of your dental provider. A skilled surgeon lowers the chance of complications.
What are the most common complications associated with dental implants?
Infection at the implant site is the most common. Other problems include implant loosening, nerve damage, and sinus issues if upper jaw implants are placed.
Most complications are rare when proper care and techniques are used.
What are the different types of dental implants and their respective costs?
There are three main types: endosteal (in the bone), subperiosteal (on the bone), and zygomatic (in the cheekbone).
Endosteal implants are the most common and usually cost between $1,500 and $3,000 per implant. Other types can be more expensive depending on complexity.
What is the step-by-step process of getting a dental implant?
First, your dentist will examine your mouth and take scans or X-rays. Then, they will place the implant post in your jawbone.
After a healing period of a few months for the bone to fuse, an abutment is added.
Finally, a crown is placed to restore your tooth’s look and function.
You will have follow-up visits to ensure the implant is stable and healthy.